Is It Folliculitis or MRSA? How to Tell the Difference
Discovering new, red, and inflamed bumps on your skin can be an unsettling experience. It immediately raises questions and concerns: is this a simple irritation, or could it be something more serious? For many, the main worry is distinguishing between a common case of folliculitis, which is the inflammation of hair follicles, and a more significant bacterial infection like MRSA. The internet can be a source of alarming and often contradictory information, which only adds to the anxiety and makes it difficult to know whether you should be concerned.
This guide is designed to cut through the confusion with calm, factual, and clinical advice. Here, you will learn the key visual differences that can help you tell folliculitis and a potential MRSA infection apart. We will clearly outline the specific warning signs-such as increasing pain, swelling, or fever-that indicate it is time to seek professional medical advice from your GP. Our goal is to provide you with the trusted information you need to assess your situation, understand your next steps, and gain peace of mind about your skin’s health.
Key Takeaways
- Understand the key differences between a common skin irritation and a potentially serious MRSA infection by comparing specific signs and symptoms.
- While most cases of folliculitis are harmless, it’s crucial to recognise that it can sometimes be caused by antibiotic-resistant bacteria.
- Identify the specific ‘red flag’ symptoms, such as fever or spreading redness, that mean you should seek professional medical advice from a GP.
- Learn why a visual check is not enough to diagnose MRSA and why a laboratory test is the only definitive way to confirm the cause of a severe skin infection.
What is Folliculitis? Understanding the Common Skin Condition
Folliculitis is a very common skin condition defined by the inflammation of hair follicles-the small pockets in your skin from which each hair grows. While its appearance can be concerning, often resembling an acne breakout or a bumpy rash, it is typically a harmless condition that resolves with simple home care. Folliculitis can be triggered by a number of factors, but the most frequent culprits are bacterial infections, friction from clothing or shaving, and sometimes yeast or fungi.
Understanding what this condition is, what it looks like, and what causes it is the first step in distinguishing it from more serious infections and finding the right path to clear skin.
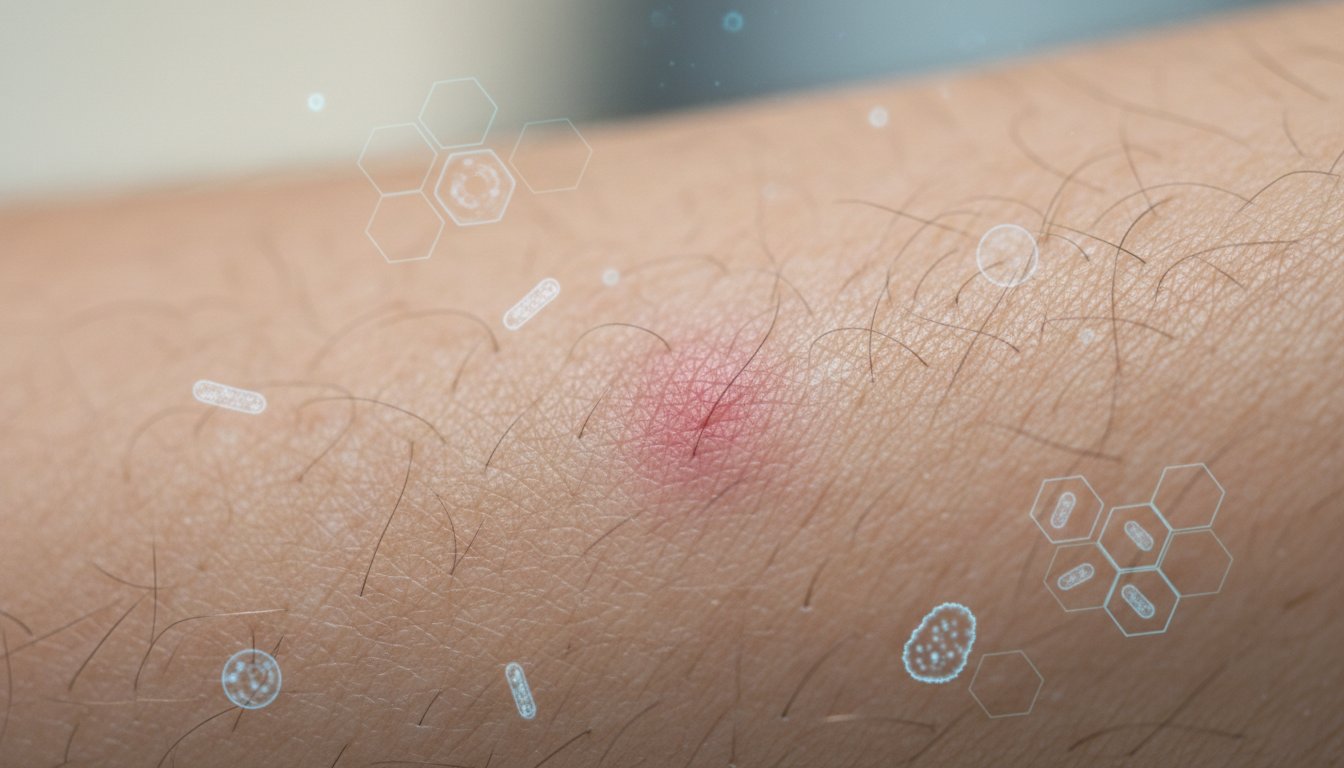
Visual Guide: What Does Folliculitis Look Like?
Folliculitis typically appears as clusters of small, red bumps or pimples with white heads that form around individual hair follicles. You may notice mild itchiness or tenderness in the affected area. It can occur anywhere on the body where hair grows but is most frequently seen on the scalp, beard area, back, chest, and legs. Unlike a single pimple, you will usually see multiple inflamed follicles in one patch of skin.
The Most Common Causes of Folliculitis
Understanding the root cause is key to both treating and preventing recurrence. The main triggers include:
- Bacterial Infection: The most common cause is the bacterium Staphylococcus aureus (Staph). This bacteria normally lives on the skin without issue but can cause an infection if it enters the body through a cut or damaged follicle.
- Mechanical Irritation: Often called ‘razor bumps’, this type is caused by friction. Shaving, waxing, or wearing tight clothing can damage hair follicles, leaving them vulnerable to inflammation.
- Environmental Factors: ‘Hot tub folliculitis’ is caused by the Pseudomonas aeruginosa bacterium, which thrives in warm, poorly maintained water like that found in some hot tubs and swimming pools in the UK.
- Fungal Infection: Known as Pityrosporum (or Malassezia) folliculitis, this type is caused by a yeast overgrowth. It often presents as itchy, acne-like bumps, particularly on the chest and back.
Folliculitis vs. MRSA: Comparing the Signs and Symptoms
Many skin infections are caused by Staphylococcus aureus (Staph) bacteria. MRSA (Methicillin-resistant Staphylococcus aureus) is a specific strain of Staph that is resistant to several common antibiotics. While Staph can cause typical folliculitis, an infection caused by MRSA can be far more severe and difficult to treat. The key is learning to recognise when a simple skin irritation has progressed into something that requires urgent medical attention.
Understanding the differences in how these infections present and progress is crucial. The table below offers a clear, side-by-side comparison of the key signs.
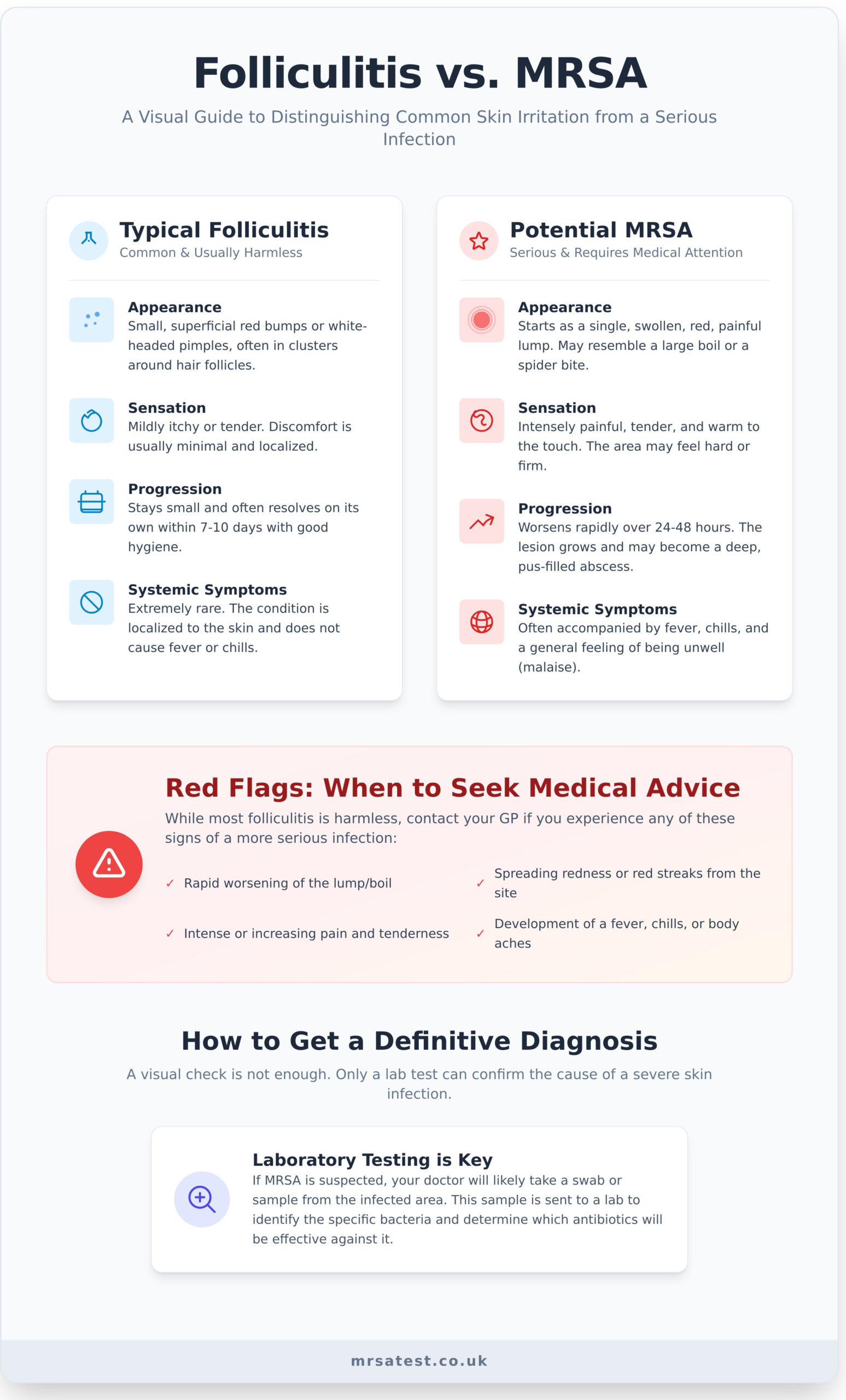
| Symptom / Feature | Typical Folliculitis | Potential MRSA Infection |
|---|---|---|
| Appearance | Small, superficial red bumps or white-headed pimples around hair follicles. Often scattered over an area. | Often starts as a single, swollen, red and painful lump. May look like a spider bite or boil. |
| Sensation | Mildly itchy or tender. Discomfort is usually minimal. | Intensely painful, tender, and warm to the touch. The area may feel hard or firm. |
| Progression | Often resolves on its own within 7-10 days. Bumps stay small. | Worsens rapidly over 24-48 hours. The lesion grows in size and pain, and may develop a pus-filled head or become a deep abscess. |
| Systemic Symptoms | Extremely rare. The infection is localised to the skin. | May be accompanied by fever, chills, and a general feeling of being unwell (malaise). |
Appearance and Progression: Key Differentiators
A standard case of folliculitis will often improve with good hygiene, whereas an MRSA infection typically worsens quickly. The lesion will grow in size, redness, and pain, often becoming a deep, pus-filled abscess. It is sometimes mistaken for an insect or spider bite in its early stages due to its isolated and inflamed appearance. As noted in medical resources on folliculitis and skin abscesses, infections caused by MRSA require prompt medical evaluation and will not resolve without proper treatment.
When to Seek Medical Advice
Perhaps the most significant warning sign is the presence of systemic symptoms. A localised skin issue should not make you feel generally unwell. If your skin lesion is accompanied by a fever, chills, or spreading redness, it is a strong indicator that the infection may be spreading. This is a characteristic of a more serious infection like MRSA and requires immediate consultation with a healthcare professional.
When to Be Concerned: Red Flags for a Serious Skin Infection
Most cases of mild folliculitis can be managed at home and will resolve on their own. However, it is crucial to recognise when a skin infection requires professional medical attention. Ignoring certain symptoms can allow a simple infection to become more serious, especially if it is caused by an aggressive bacteria like MRSA. If you notice any of the following signs, it is essential to contact your GP or seek medical advice promptly.
Key Warning Signs to Watch For
While a few small, pimple-like bumps are typical, be alert for signs that the infection is worsening. Do not delay seeking help if you experience:
- Spreading Redness: The area of red, inflamed skin around the bumps is growing quickly in size.
- Severe or Worsening Pain: The discomfort is more than just mild tenderness and is intensifying over time.
- Systemic Symptoms: You develop a fever, chills, or feel generally unwell and fatigued, which indicates the infection may be spreading.
- Large Boils (Furuncles): A single infected follicle develops into a large, painful, pus-filled lump. If several of these merge, they form an even larger cluster called a carbuncle.
Who is at Higher Risk for MRSA?
While anyone can get MRSA, certain factors increase your risk of exposure to this antibiotic-resistant bacteria. This is particularly important if your skin infection is not responding to initial treatment. Key risk factors include:
- Recent hospitalisation, surgery, or a stay in a long-term care facility.
- Participation in close-contact sports, such as rugby or wrestling.
- Living in crowded or shared environments like university halls or military barracks.
- Having a compromised immune system due to a medical condition or medication.
Why You Should Never Squeeze a Boil
It can be tempting to squeeze a boil to release the pus, but this is a dangerous mistake. Squeezing applies pressure that can rupture the infection deep under the skin, forcing bacteria further into your tissues and potentially into your bloodstream. This action can worsen the infection, lead to severe scarring, and spread the bacteria to other parts of your body or to other people. A healthcare professional can determine if drainage is necessary and perform it safely in a sterile environment. The process for Diagnosing folliculitis and related infections may involve a physical exam or a culture to identify the bacteria, ensuring you receive the correct treatment.
How to Get a Definitive Diagnosis
While many skin bumps look similar, it’s impossible to distinguish a severe case of bacterial folliculitis from an MRSA infection just by looking. Even for a trained medical professional, a visual assessment is not enough for a definitive answer. The only way to know for certain is through a laboratory test that identifies the specific bacteria causing the infection and checks for antibiotic resistance.
Seeing a Healthcare Professional
If you visit a GP or dermatologist, they will begin with a physical examination of the affected skin and ask about your symptoms and medical history. If an infection like MRSA is suspected, they will typically take a swab of pus or fluid from the boil or abscess. This sample is then securely sent to a laboratory for analysis to confirm the cause.
Understanding Lab Tests: Culture vs. PCR
Once at the lab, your sample will be analysed using one of two highly accurate methods to identify the bacteria:
- Culture Test: This traditional method involves placing the sample in a special medium to encourage bacterial growth. Technicians can then identify the specific strain of Staphylococcus aureus and test its sensitivity to various antibiotics. Results are typically available in 2-3 days.
- PCR Test: A Polymerase Chain Reaction (PCR) test is a rapid molecular method that detects the specific DNA of the MRSA bacteria. It offers much faster results, often within 24 hours, by directly identifying the genetic markers of the organism.
Both methods are the gold standard for confirming an MRSA infection and guiding effective treatment.
Confidential At-Home MRSA Screening
For non-urgent concerns, pre-surgery screening, or for those who simply want peace of mind, a confidential at-home test is a convenient and reliable alternative. The process is designed to be simple and completely discreet. You order a kit online, collect a sample using a simple, painless swab, and post it back to our UKAS-accredited partner laboratory in the pre-paid packaging provided. This allows you to test for MRSA from the comfort of your own home, ensuring privacy and accuracy. Get peace of mind with a confidential at-home MRSA test.
General Advice for Managing and Preventing Folliculitis
Understanding how to manage mild skin inflammation and prevent its recurrence is a key part of maintaining skin health. While many simple cases can be managed at home, it is essential to distinguish between general advice and specific medical treatment. Please note: the following guidance is intended for managing and preventing uncomplicated, superficial folliculitis. It is not a treatment plan for a diagnosed or suspected MRSA infection. An MRSA infection is a serious medical condition that requires prompt diagnosis and treatment from a healthcare professional.
Home Care for Mild Cases
For minor, superficial cases that are not causing significant pain or spreading, these simple measures can help soothe irritation and promote healing. If symptoms do not improve within a few days, consult a healthcare provider.
- Apply warm compresses: Soaking a clean washcloth in warm water and applying it to the affected area for 15-20 minutes, several times a day, can help reduce discomfort and encourage any trapped fluid to drain.
- Keep the area clean: Gently wash the inflamed skin twice daily with an antibacterial soap and warm water. Pat the area dry with a clean towel; do not rub, as this can worsen irritation.
- Avoid shaving or waxing: Refrain from shaving, waxing, or plucking hair in the affected area until the inflammation has completely subsided. This prevents further irritation and reduces the risk of spreading bacteria.
- Wear loose-fitting clothing: Tight clothing can trap heat and moisture while causing friction against the skin. Opt for loose, breathable fabrics like cotton to keep the area dry and minimise irritation.
Prevention Strategies
Adopting consistent hygiene practices is the most effective way to reduce your risk of developing folliculitis in the future. These habits help to minimise the presence of bacteria on the skin and prevent irritation to hair follicles.
- Practice good personal hygiene: Shower promptly after exercising or sweating heavily to wash away bacteria and oils that can clog follicles. Use a clean towel every time you bathe.
- Avoid sharing personal items: Bacteria can easily transfer between individuals. Never share items such as towels, razors, washcloths, or bars of soap.
- Use clean pools and hot tubs: Only use facilities that are well-maintained. “Hot tub folliculitis” is caused by bacteria that thrive in improperly treated warm water.
- Shave with care: Use a clean, sharp blade each time you shave. Apply a lubricating shaving cream or gel, and always shave in the direction of hair growth, not against it.
In addition to these hygiene practices, some people also look into alternative health modalities for supporting overall wellness and resilience against infections. If you’re interested in learning about emerging approaches like bio-electric therapy, you can check out Electronic Kit Complete.
Ultimately, the key difference between managing a simple skin irritation and addressing MRSA lies in the need for an accurate diagnosis. If your symptoms are severe, persistent, or you are concerned about potential exposure, seeking professional medical advice is the most responsible step. For confidential confirmation, you can test for MRSA from the comfort of your own home.
Your Path to a Clear Diagnosis and Peace of Mind
Understanding your skin is the first step towards effective treatment. While many red bumps are simply benign folliculitis, some symptoms can overlap with more serious conditions like MRSA. Recognising the key differences and knowing when to seek professional advice is crucial, but for complete certainty, a definitive diagnosis is the only way to ensure you receive the appropriate care.
If you have any concerns about a persistent or severe skin infection, taking proactive steps is the best course of action. Don’t let uncertainty cause you anxiety. For confidential and reliable screening from the comfort of your home, you can Order Your Confidential At-Home MRSA Test Kit Today.
Our service ensures complete privacy with discreet packaging and delivery. Your sample will be processed in a UKAS-accredited laboratory, with both rapid PCR and standard culture options available to provide you with fast, accurate results you can trust. Taking control of your health is a powerful step, and with a clear answer, you can move forward with confidence.
Frequently Asked Questions
Can simple folliculitis turn into MRSA?
Simple folliculitis does not transform into MRSA. Folliculitis is the inflammation of hair follicles, which can be caused by various bacteria. MRSA is a specific, antibiotic-resistant strain of the Staphylococcus aureus bacterium that can cause folliculitis. Therefore, an infection is either caused by MRSA from the outset, or it is caused by a different, non-resistant bacterial strain. An infection from a non-resistant strain cannot change into an MRSA infection.
Is bacterial folliculitis contagious?
Yes, bacterial folliculitis can be contagious. The bacteria responsible, such as Staphylococcus aureus, can spread through direct skin-to-skin contact with an infected person. It can also be transmitted indirectly by sharing personal items that have touched the infected area, including towels, razors, flannels, and bedding. Maintaining good personal hygiene is crucial to prevent spreading the infection to others or to other parts of your own body.
How long does it take for mild folliculitis to go away on its own?
In many cases, mild folliculitis will resolve by itself with consistent home care. You can typically expect the condition to clear up within 7 to 10 days. Applying warm compresses to the affected skin and keeping the area clean can help soothe discomfort and encourage healing. If the condition persists beyond two weeks, worsens, or becomes very painful, it is advisable to seek guidance from a healthcare professional for an accurate diagnosis.
What does an early-stage MRSA skin infection look like?
An early-stage MRSA skin infection often begins as a red, swollen, and painful bump on the skin, which can easily be mistaken for a common spot, insect bite, or small boil. The area may feel warm to the touch and can develop a head containing pus or other fluid. Unlike a simple pimple, an MRSA lesion can rapidly grow larger and more painful. Any suspicious skin lesion that worsens quickly warrants prompt medical attention.
Should I get tested for MRSA if I get recurring boils or abscesses?
Yes, if you experience recurrent boils or abscesses, getting tested for MRSA is a highly recommended step. Persistent or recurring skin infections are a key indicator that you may be colonised with MRSA, where the bacteria live on your skin without causing illness but can lead to repeated infections. A definitive diagnosis through a screening test allows for targeted and effective management, helping to break the cycle of recurrence and provide clear answers.
Can you have MRSA on your skin without having an active infection?
Yes, it is entirely possible to carry MRSA bacteria on your skin or in your nose without any signs or symptoms of an infection. This is referred to as being “colonised” or being a carrier. A colonised individual is typically healthy but can potentially spread the bacteria to others who may be more vulnerable to infection. Screening is the only reliable method to determine if you are an MRSA carrier, which is vital information before a hospital procedure.