What Does an MRSA Rash Look Like? A Visual and Clinical Guide
Imagine noticing a small, red bump on your arm that you dismiss as a common spider bite, only to find it becoming increasingly painful and swollen within 24 hours. According to clinical data, around 1 in 30 people in the UK carry MRSA on their skin or in their nose without even knowing it, making it easy to mistake a serious infection for a minor irritation. Many patients only begin to search for what does an mrsa rash look like once a bump starts to resemble a boil or begins to produce pus.
It’s natural to feel anxious when a skin condition doesn’t behave as expected, especially when you’re concerned about protecting your household from infection. We understand that you need clear, factual information to alleviate this worry and regain your peace of mind. This guide provides a clinical framework to help you identify the specific visual warning signs of an MRSA skin infection and distinguish it from common rashes. We will walk you through the progression of symptoms, explain how to access discreet, UKAS-accredited testing, and clarify exactly when you should contact your GP or seek emergency care.
Key Takeaways
- Understand why MRSA is often misidentified as a simple skin irritation and learn how to recognize it as a localized lesion rather than a common flat rash.
- Discover what does an mrsa rash look like by identifying the hallmark “spider bite” appearance and the specific textures that indicate a deep bacterial infection.
- Learn how to distinguish aggressive MRSA abscesses from common skin mimics like folliculitis to ensure you seek the correct clinical intervention.
- Identify the life-threatening systemic symptoms and the “Glass Test” results that signal a medical emergency requiring immediate 999 or A&E attention.
- Find out why visual checks are never enough for a definitive diagnosis and how to access professional UKAS-accredited laboratory testing from home.
Understanding the MRSA “Rash”: Is It Actually a Rash?
When people ask what does an mrsa rash look like, they’re often surprised to learn that it rarely resembles a typical skin rash. Unlike eczema or heat rash, which spread across the skin in flat, red patches, Methicillin-resistant Staphylococcus aureus (MRSA) usually presents as a distinct lesion, sore, or abscess. It’s a type of staph bacteria that’s evolved to resist standard antibiotics like methicillin and penicillin. This resistance makes it a “superbug,” as common treatments don’t clear the infection, often leading to more severe symptoms if left unmanaged.
It’s vital to distinguish between being colonized and having an active infection. Data suggests that around 2% of the UK population carries MRSA on their skin or in their nose without showing any symptoms. This is known as colonization. An infection only occurs when the bacteria multiply and cause tissue damage, leading to the visible sores people often mistake for a rash. Because these bacteria are resilient, identifying the signs early is the best way to ensure you receive the correct clinical care.
The Definition of an MRSA Skin Infection
An MRSA skin infection is a localized inflammatory response caused by staph bacteria that have developed resistance to common penicillin-based antibiotics. These bacteria typically enter the body through microscopic breaks in the skin, such as small cuts, grazes, or even through hair follicles. Medical professionals generally categorise these infections into two types. Hospital-acquired (HA-MRSA) typically affects patients in clinical settings, while community-acquired (CA-MRSA) spreads through close contact or shared items in places like gyms or schools.
Why People Mistake Infections for Rashes
The term “rash” is frequently used because, in its very early stages, an MRSA infection can appear as a cluster of small, red bumps. These clusters might look like hives or heat rash at first glance. However, the key difference lies in how the area feels. While a standard rash might just change the surface colour of your skin, an MRSA lesion feels firm, warm, and tender to the touch. Instead of being a surface irritation, it’s an internal battle between your immune system and the bacteria. Understanding what does an mrsa rash look like involves looking for localized swelling and pain rather than just a flat change in skin tone.
- Texture: MRSA sores often feel like a hard lump under the skin.
- Progression: Unlike a rash that stays flat, MRSA lesions often quickly turn into pus-filled boils.
- Sensation: The area is typically painful and may throb, which isn’t common with standard rashes.
Visual Symptoms: What Does MRSA Look Like on the Skin?
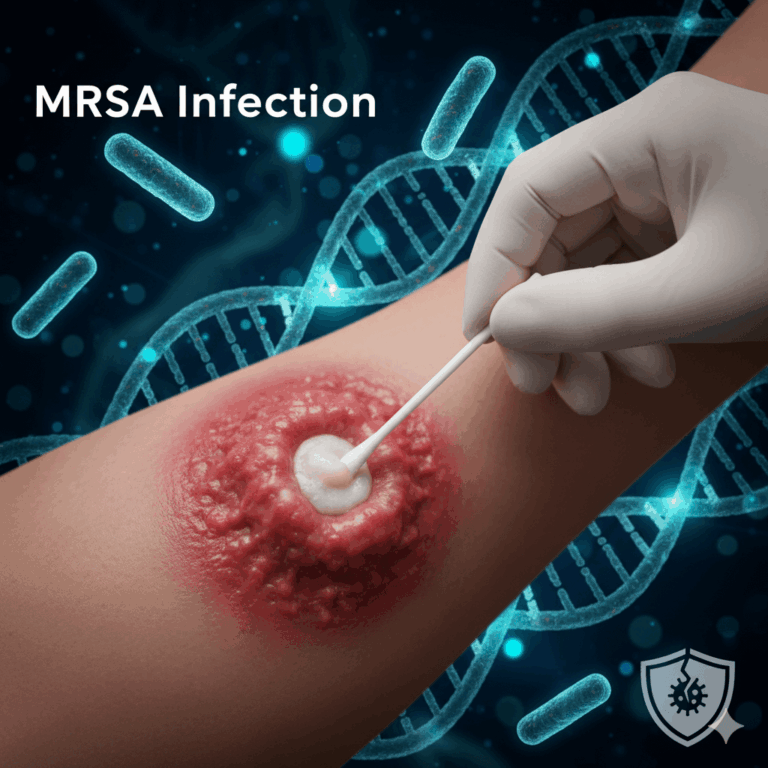
When patients first ask what does an mrsa rash look like, they often describe a sudden, painful bump that they mistake for a spider bite. This “spider bite” appearance is a hallmark of a Methicillin-resistant Staphylococcus aureus (MRSA) skin infection. The site typically presents as a swollen, red, and tender area that can quickly escalate in severity. Unlike a typical pimple, an MRSA lesion often feels hard to the touch, almost like a firm “knot” or a marble buried just beneath the surface of the skin.
Clinical observation usually reveals a collection of pus or clear fluid at the centre of the bump. As the infection develops, this may leak or form honey-coloured scabs, a sign often associated with staphylococcal activity. A critical diagnostic sign is the temperature of the skin. The area surrounding the lesion will feel significantly warmer than the rest of your body. This localized heat indicates that your immune system is actively fighting an inflammatory process. Key indicators to watch for include:
- A localized bump that mimics a persistent insect bite.
- Skin that feels firm, tight, or “knotted” underneath.
- Intense heat radiating from the specific site of the bump.
- Yellow or white pus drainage or crusting.
Identifying MRSA on Different Skin Tones
Identifying MRSA on different skin tones requires a focus on tactile changes rather than just colour. On brown or black skin, the classic “redness” might not be obvious. Instead, the infected area may appear dark brown, purple, or even grey and pale. Because visual cues are subtle, medical professionals rely on feeling for firmness and swelling. If a patch of skin feels unusually thick, hard, or hot to the touch, it warrants immediate attention, even if no redness is visible. Understanding what does an mrsa rash look like on diverse skin types ensures that the infection isn’t overlooked in its early stages.
The Progression of a Lesion
The timeline of an MRSA lesion usually begins with a small, pimple-like irritation. Within 24 to 48 hours, this can transform into a deep, painful abscess. You should watch for red streaks extending from the site. This is a clinical sign that the infection is moving into the lymph system and requires urgent medical review. During the “weeping” stage, the lesion may break open and drain. This fluid is highly contagious and contains high concentrations of the bacteria. Following MRSA testing and prevention in the UK guidelines is vital at this stage to stop the spread to others. If you’re concerned about a recurring skin issue, you can order a discreet home screening kit to get clear, professional answers from the comfort of your home.

Differential Diagnosis: MRSA vs. Common Skin Mimics
Identifying a skin infection accurately is the first step toward effective treatment. Many patients struggle to determine what MRSA looks like because it shares characteristics with several benign conditions. While a standard MRSA infection often presents as a localized, painful boil, other issues like cellulitis cause widespread skin redness without a defined “head” or point of drainage. To help you distinguish between these possibilities, we provide a visual guide to common skin infections that illustrates these differences through clinical comparisons.
Distinguishing MRSA from common mimics is vital for your safety. When asking what does an mrsa rash look like, it is helpful to look for a “central point” or abscess. Unlike a simple rash, MRSA usually feels like a firm, warm lump under the skin. It lacks the widespread, flat appearance of a typical allergic reaction or heat rash. If the area is expanding rapidly or is accompanied by a fever, it suggests a bacterial invasion rather than a simple irritation.
MRSA vs. Folliculitis and Cysts
MRSA frequently begins its invasion within a hair follicle. This initial stage mimics folliculitis, which appears as small, itchy, red bumps. However, while standard folliculitis usually resolves on its own, MRSA progresses into a deep, warm abscess. You should never attempt to squeeze or “pop” a suspected MRSA bump. Squeezing forces the Staphylococcus aureus bacteria deeper into your soft tissue or bloodstream; this can lead to life-threatening complications. In contrast, sebaceous or ganglion cysts are typically slow-growing and painless, whereas MRSA is aggressive and tender to the touch.
The “Spider Bite” Myth
In the UK, many patients mistakenly attribute a sudden, painful lesion to a spider bite. Data from the Natural History Museum indicates that only about 12 of the 650 spider species in the UK can actually bite humans, and even fewer cause significant reactions. If you notice a lesion that is getting worse after 48 hours, it’s likely bacterial. Use this checklist to evaluate the area:
- Presence of Pus: Does the lesion have a visible “head” or drainage?
- Rapid Progression: Is the redness spreading or becoming more painful each hour?
- Systemic Symptoms: Do you have a fever, chills, or general malaise?
Understanding your specific risk factors is vital for an accurate diagnosis. You can find more detail in our complete guide to MRSA symptoms to see if your lifestyle or health history increases your vulnerability to this specific pathogen.
When an MRSA Rash Becomes an Emergency
Identifying what does an mrsa rash look like is a vital first step in managing your health, but you must also recognize when a skin issue evolves into a systemic threat. While many staph infections remain localized, MRSA is resilient. If the bacteria bypass the skin’s barrier and enter the bloodstream, the situation changes from a dermatological concern to a medical emergency. You should never ignore a non-healing wound, especially if it remains open or continues to weep after 10 days of standard care.
One critical diagnostic tool you can use at home is the “Glass Test.” Press a clear drinking glass firmly against the rash or red spots. If the marks do not fade or “blanch” under the pressure, it indicates bleeding under the skin. This non-blanching rash is a major red flag for sepsis or a serious systemic reaction. If you see this, or if a red line begins to streak away from the site of the infection, you must contact 999 or attend your nearest A&E department immediately.
For individuals with weakened immune systems, the risks are even higher. A minor lesion that looks like a typical spot can quickly escalate. Monitoring the site daily is essential; any rapid spreading or a sudden increase in pain levels requires professional clinical intervention to prevent the bacteria from reaching the bones or vital organs.
Signs of Systemic Infection (Sepsis)
When the infection spreads beyond the initial site, you may experience a “shivering” sensation or a sudden onset of flu-like symptoms. This is often the body’s first response to the bacteria entering the blood. Critical red flags include confusion, extreme dizziness, and a rapid heart rate that doesn’t slow down when you rest. You might also notice your skin feels cold or clammy to the touch. While MRSA is treatable with the correct intravenous antibiotics, delays in systemic cases can be life-threatening. Early detection of these “whole-body” symptoms is the most important factor in a successful recovery.
The Role of Pre-Op Screening
Hospitals in the UK routinely screen patients for MRSA because the bacteria often live harmlessly on the skin or in the nose without causing any visible symptoms. This is known as colonization. However, when a surgeon makes an incision, that dormant colonization can move inside the body, leading to a serious surgical site infection. Understanding preparing for surgery involves more than just logistical planning; it requires clinical certainty that you aren’t carrying the bacteria into the operating theatre.
Many patients choose private screening before elective procedures for total peace of mind. Using a UKAS-accredited facility ensures that your results are accurate and reliable. Knowing your status beforehand allows you to undergo simple decolonization treatments, such as antiseptic body washes and nasal creams, which significantly reduces the risk of post-operative complications. It’s a proactive step that ensures your recovery is as smooth and safe as possible.
If you are concerned about a persistent skin change or need clearance for an upcoming procedure, order a discreet MRSA home test kit today for fast, professional results.
Proactive Management: Testing and Prevention in the UK
Identifying what does an mrsa rash look like is a useful first step, but visual assessment is never 100% accurate. Many common skin infections, such as simple cellulitis or spider bites, mimic the appearance of MRSA. To be certain, you need a clinical swab test. This is the only way to confirm if the bacteria present are resistant to methicillin, which dictates the type of antibiotics required for treatment.
Using a UKAS-accredited laboratory ensures your sample is handled with clinical precision. These facilities follow strict UK regulations to provide reliable, accurate data that you can trust. For those who aren’t showing symptoms but belong to high-risk groups, such as individuals preparing for hospital admission or those living with vulnerable people, proactive screening is essential. You can access MRSA test kits for fast, discreet results without needing an immediate GP appointment.
How At-Home MRSA Testing Works
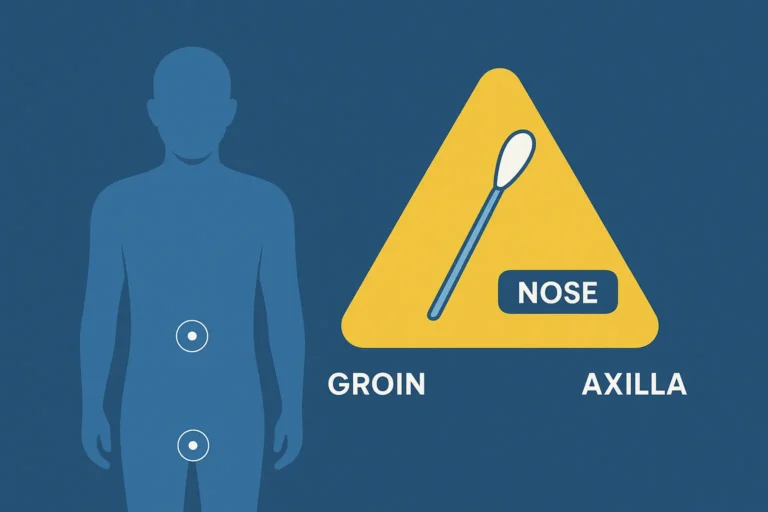
The testing process is designed to be simple and stress-free. You’ll use sterile swabs to collect samples from three primary areas: the nose, the groin, and the axilla (armpit). These are the most common sites where MRSA bacteria colonise the skin. Once you’ve collected the samples, you post them back to our 100% UK-based partner laboratory.
You can choose between a standard Culture test or a Rapid PCR test. The PCR option provides molecular detection in just 24 hours once the lab receives your sample, making it ideal for urgent screening. Every kit is delivered in plain packaging to maintain your privacy. Results are delivered through a confidential digital portal, ensuring your health data stays secure and private at all times.
Preventing the Spread at Home
If you’re concerned about infection or have confirmed colonization, following a strict hygiene protocol is vital to protect others in your household. Start with these three essential steps:
- Wash your hands: Use soap and water or alcohol-based sanitiser frequently, especially after touching a wound.
- Cover the wound: Keep any active sores or rashes covered with clean, dry bandages until they’ve fully healed.
- Don’t share: Stop sharing personal items like towels, razors, or bed linens with other family members.
If a test confirms you’re colonized, a healthcare professional might recommend chlorhexidine (CHG) washes. These specialized antiseptic cleansers help reduce the bacterial load on your skin and are a standard part of decolonization therapy. Using at-home test kits in the UK is a valid first step in taking control of your health and stopping the spread of resistant bacteria before it becomes a larger issue.
Take Proactive Steps for Your Skin Health
Identifying what does an mrsa rash look like is the first step toward effective management. While it often mimics a common spider bite or a painful boil, MRSA requires specific clinical attention to prevent the infection from spreading. If you’ve noticed a red, swollen area that’s warm to the touch or producing pus, getting an accurate diagnosis is essential for your peace of mind. You don’t have to navigate these concerns alone or wait for a GP appointment.
Our service provides a professional and efficient way to screen for colonization from the comfort of your own home. We process all samples in UKAS-accredited UK laboratories to ensure the highest clinical standards. Every order includes discreet, plain-packaged shipping and collection, so your privacy remains a top priority throughout the process.
Order a Confidential MRSA Home Test Kit with 24-Hour Results to access rapid PCR testing. You’ll receive your results within 24 hours of our laboratory receiving your sample. Taking charge of your health is a simple, secure, and vital step toward your recovery.
Frequently Asked Questions
Can MRSA look like a pimple?
Yes, MRSA often begins as a small, red, swollen bump that closely resembles a common pimple or a whitehead. Because the bacteria frequently enter through a hair follicle, the initial lesion may look like standard folliculitis. If the bump is unusually painful, firm, or warm to the touch, it’s likely more than a standard blemish and requires professional attention.
How quickly does an MRSA rash spread?
An MRSA infection can spread and worsen significantly within 24 to 48 hours. What starts as a minor irritation can quickly develop into a deep, painful abscess or cellulitis. Clinical data suggests that prompt identification is vital, as the infection can bypass the skin barrier and enter the bloodstream or internal organs if ignored for more than 3 days.
Is an MRSA rash itchy or painful?
Most patients report that an MRSA rash is significantly more painful than it is itchy. While you might feel a slight itch as the skin stretches, the primary symptoms are tenderness, heat, and a throbbing sensation. If you are wondering what does an mrsa rash look like, look for intense redness that covers a 2 to 5 centimetre area around the central point.
What does MRSA look like when it starts to heal?
When MRSA begins to heal after successful antibiotic treatment, the intense redness and swelling will start to subside within 3 to 5 days. Any active drainage or pus will dry up; a firm scab will then form over the site. The skin temperature around the infection will return to normal as the inflammation resolves, though some scarring or dark pigmentation may remain for several months.
Can I test for MRSA at home if I have a suspicious bump?
You can certainly test for MRSA from the comfort of your own home using a professional screening kit. Our service provides a discreet, UKAS-accredited MRSA culture test that uses a simple swab method to detect colonisation. This allows you to get accurate results without a GP appointment; samples are processed in a trusted UK partner laboratory to ensure clinical standards.
Does MRSA always produce pus?
MRSA does not always produce pus, though it is present in approximately 75% of skin-based infections. In cases of MRSA-related cellulitis, the skin becomes flat, red, and swollen without a defined head or pocket of fluid. However, if an abscess forms, it will typically be filled with white, yellow, or green fluid as the body tries to fight the bacterial invasion.
What should I do if I think my “spider bite” is actually MRSA?
If you suspect a “spider bite” is actually MRSA, you should cover the area with a sterile bandage and avoid the urge to squeeze it. True spider bites are rare in the UK, whereas MRSA is a common cause of sudden, painful skin lesions. Seek a professional screening or visit a clinician if the area develops a black centre or if you develop a fever over 38°C.
How do I know if my MRSA infection is contagious?
An MRSA infection is contagious as long as the bacteria are active on the skin or present in wound drainage. To understand what does an mrsa rash look like when it’s most infectious, look for any open sores or weeping fluid. You can reduce the risk of transmission by washing your hands for 20 seconds with antibacterial soap and not sharing towels or razors with others.