A Visual Guide to Common Skin Infections: Types, Symptoms & When to See a Doctor
A new rash, sore, or unusual patch of skin can be a source of immediate concern. You may be wondering: Is it contagious? Will it go away on its own? Or could it be something more serious? Navigating the world of common skin infections can feel overwhelming, especially with the volume of conflicting information available online.
This visual guide is designed to provide clarity and reassurance. We will break down the key differences between the three primary types of skin infections-bacterial, viral, and fungal. Using clear descriptions and visual examples, you will learn to identify potential symptoms, understand their likely causes, and gain a better understanding of their potential severity.
Most importantly, this guide will help you determine the crucial next step: whether your condition can be managed at home or if it requires professional medical advice from a GP. Our aim is to equip you with trusted information so you can approach your skin health with confidence and clarity.
Key Takeaways
- Understanding the cause of a skin infection-whether bacterial, viral, or fungal-is the first step towards receiving effective treatment.
- Learn to recognise the key visual differences between common skin infections, helping you to distinguish between various types of rashes, sores, and blisters.
- Identify the specific symptoms, such as a high fever or rapidly spreading redness, that indicate it is time to consult your GP for a professional diagnosis.
- Gain clarity on the diagnostic process and why the correct treatment, such as antibiotics for bacteria or antifungals for fungi, is crucial for recovery.
Understanding the Four Main Types of Skin Infections
Your skin is your body’s first line of defence, a remarkable barrier against the outside world. However, when this barrier is compromised by a cut, scrape, or even a microscopic break, it can become an entry point for microorganisms. This is how most common skin infections begin. Understanding the cause is the first step toward effective treatment, as infections are typically caused by one of four main culprits: bacteria, viruses, fungi, or parasites. While many skin conditions are highly treatable, correct identification is crucial for selecting the right approach. These pathogens are broadly categorised into four groups, leading to different Types of Skin Infections, each with distinct characteristics.
Bacterial Infections
Bacterial infections occur when bacteria, such as Staphylococcus, enter the skin, often through a break or a blocked hair follicle. They typically present as red, swollen, and often painful bumps, sores, or abscesses. These infections can range from mild, superficial conditions like impetigo, which is common in children, to more severe infections like cellulitis, which affects deeper layers of the skin and requires prompt medical attention.
Viral Infections
Caused by viruses, these infections can be localised to one area or spread more widely across the body. The appearance of viral skin infections varies significantly. Examples include the rough, bumpy growths of warts (caused by the human papillomavirus), the painful blisters of cold sores (herpes simplex virus), and the distinctive rash of shingles. While some viral conditions may resolve on their own, others require specific antiviral medications to manage symptoms and prevent spread.
Fungal Infections
Fungal infections, or mycoses, are caused by fungi that thrive in warm, damp environments. This makes areas like the feet, groin, and skin folds particularly susceptible. Common examples include athlete’s foot, jock itch, and ringworm (which, despite its name, is a fungus). These conditions typically appear as scaly, red, and intensely itchy patches, sometimes forming a ring-like shape. Many are effectively treated with over-the-counter antifungal creams or powders available from a pharmacy.
Parasitic Infections
Parasitic infections are caused by tiny organisms that live on or burrow into the skin to feed and lay eggs. The primary symptom is almost always intense itching, which can be particularly severe at night. Well-known examples in the UK include scabies, caused by a microscopic mite, and head lice. Unlike other common skin infections, these cannot be treated with general antibiotics or creams and require specific prescribed medications to eliminate the parasites and their eggs completely.
A Closer Look at Common Bacterial Skin Infections
Bacterial infections are among the most frequent types of common skin infections, often caused by bacteria that are normally present on our skin, such as Staphylococcus and Streptococcus. When these microbes breach the skin’s protective barrier through a cut or graze, they can multiply and cause an infection. The appearance can vary significantly, from small, pus-filled pustules to large, inflamed red areas. Prompt diagnosis and treatment are essential to prevent the infection from spreading or becoming more severe.
Cellulitis
Cellulitis is a bacterial infection that affects the deeper layers of the skin and the fat tissue beneath. It typically appears as a red, swollen area that feels warm and tender to the touch. The affected area of redness often expands rapidly, and the infection can sometimes be accompanied by a fever. Because cellulitis can lead to more serious complications if left untreated, it requires prompt medical attention and a course of oral antibiotics.
Impetigo
A highly contagious skin infection, impetigo is particularly common in young children. It usually begins as small red sores, often around the nose and mouth, which then burst and develop distinctive honey-coloured crusts. Impetigo is spread through direct contact with the sores or contaminated items like towels. Treatment is straightforward and typically involves either a topical antibiotic cream or, for more widespread cases, oral antibiotics to clear the infection.
Folliculitis
Folliculitis is the inflammation of hair follicles, which can result in a rash of small, pimple-like bumps that may have a white head. It can be caused by a bacterial infection but is also triggered by friction from clothing, shaving, or blocked follicles. While it can appear anywhere there is hair, it is most common on the beard area, arms, legs, and buttocks. Mild cases of folliculitis often resolve on their own with improved skin hygiene.
Choosing well-fitting clothing made from breathable fabrics can help minimize such friction and irritation. For those looking to invest in high-quality, comfortable wardrobe staples, resources from brands like Urban Mave can offer helpful guidance.
Staphylococcus aureus and the Rise of MRSA
Staphylococcus aureus, often shortened to ‘staph’, is a bacterium commonly found on the skin or in the nose of many healthy individuals. While usually harmless, it can cause infections if it enters a wound. A particular concern is MRSA (Methicillin-resistant Staphylococcus aureus), a strain of staph that has developed resistance to several common antibiotics. Professional guidance on Diagnosing and Treating Skin Infections highlights the importance of identifying the correct bacteria to ensure effective treatment. An MRSA infection can initially look like a simple spider bite or pimple but can quickly become a serious abscess. Concerned it might be MRSA? See how to identify an MRSA rash.
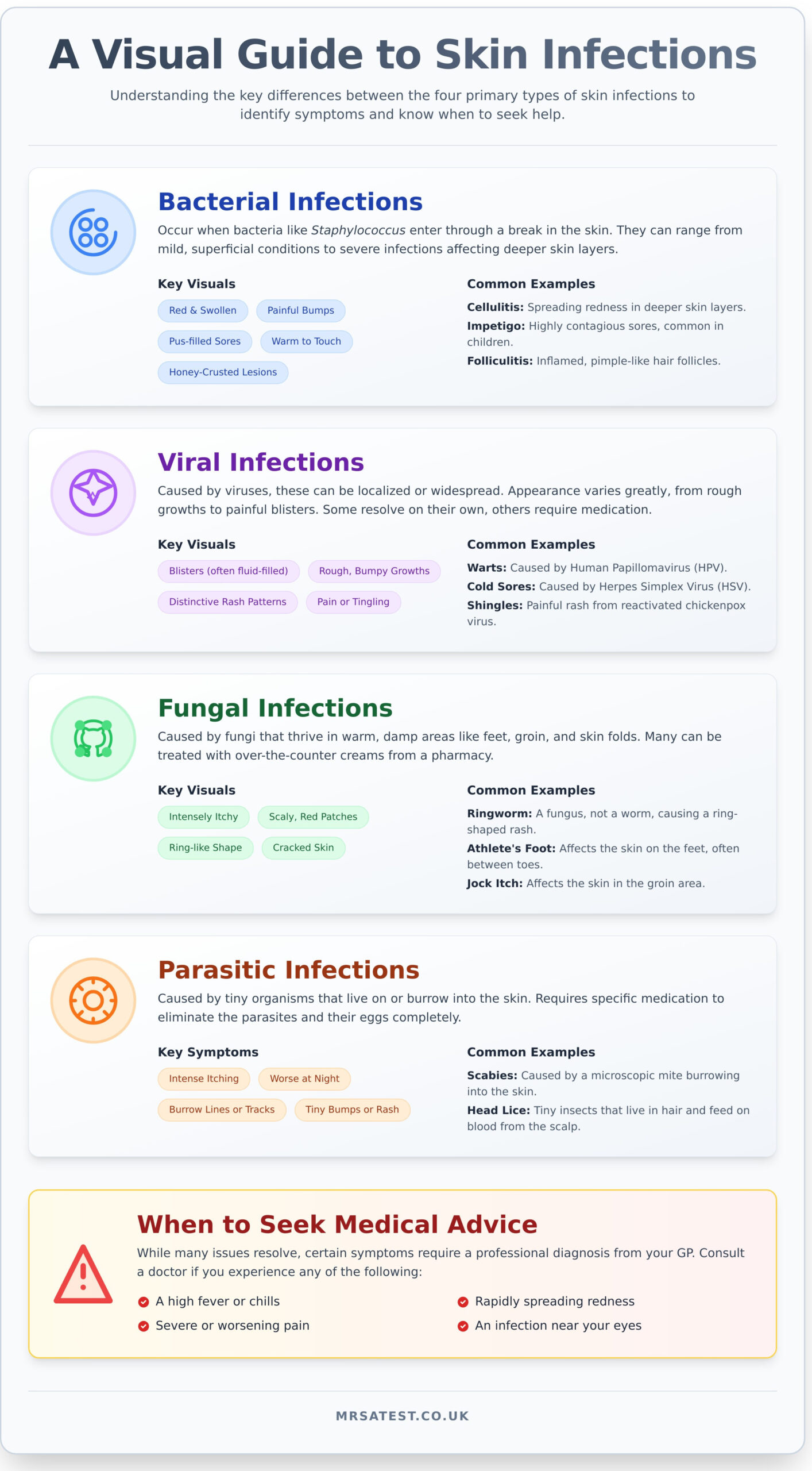
Identifying Common Viral and Fungal Skin Infections
Unlike bacterial infections, viral and fungal conditions do not respond to antibiotics, making accurate identification crucial for effective treatment. Understanding the visual differences between these common skin infections is the first step. Viral infections often present as distinct blisters or growths, while fungal infections typically manifest as superficial, itchy, and scaly rashes. Below is a guide to help you distinguish between some of the most frequently encountered types.
Ringworm (Tinea)
Despite its misleading name, ringworm is not caused by a worm but by a common fungus. It is highly contagious and can be passed through direct contact or by touching contaminated surfaces. Its appearance is highly characteristic, making it relatively easy to identify.
- Visual Cue: The classic sign is a circular, red, and scaly rash with a raised border, often resembling a ring. The centre of the ring may appear clear.
- Location: It can appear anywhere on the body (tinea corporis), scalp (tinea capitis), or feet, where it is known as athlete’s foot (tinea pedis).
- Treatment: Most cases can be managed effectively with over-the-counter antifungal creams, sprays, or powders available from your local chemist.
Warts (Verrucae)
Warts are harmless skin growths caused by an infection with the human papillomavirus (HPV). While they can appear anywhere, they are most commonly found on the hands and feet. They are contagious and can spread through direct skin-to-skin contact.
- Visual Cue: Warts are typically small, grainy bumps that feel rough to the touch. They may contain tiny black dots, which are clotted blood vessels.
- Location: Common warts often grow on fingers and hands. Plantar warts, or verrucas, develop on the soles of the feet and can be painful when walking.
- Treatment: Many warts disappear without treatment, but this can take months or years. Over-the-counter preparations or professional removal by a GP may be required for persistent cases.
Cold Sores (Herpes Simplex Virus)
Also known as fever blisters, cold sores are caused by the herpes simplex virus (HSV-1). Once you have the virus, it remains dormant in your nerve cells and can be reactivated periodically throughout your life. These outbreaks are often predictable and follow a distinct pattern.
- Visual Cue: They appear as small, painful, fluid-filled blisters, typically in a cluster on or around the lips. The blisters will eventually burst, crust over, and heal.
- Triggers: Common triggers for an outbreak include stress, fatigue, illness (like a cold or flu), or prolonged exposure to sunlight.
- Treatment: There is no cure for the virus, but antiviral creams can help ease symptoms and speed up the healing time of an outbreak.
When to See a Doctor About a Skin Infection
Many mild or common skin infections can be managed effectively at home with basic first aid and over-the-counter treatments. However, knowing when to seek professional medical advice is crucial for preventing complications and ensuring a swift recovery. Trusting your judgment is important; if a skin issue feels wrong or is causing you concern, a professional opinion provides peace of mind and the correct course of action.
Monitoring the site of a potential infection is a key step in self-care. While the body is adept at healing, certain signs indicate that it may be struggling to control the spread of bacteria or fungi.
Consult Your GP if You Experience:
While not necessarily an emergency, certain symptoms indicate that a professional diagnosis and treatment, such as prescription antibiotics, are required. It is advisable to book an appointment with your GP if you notice any of the following:
- A persistent sore: The affected area is not healing, is slowly getting larger, or has not improved after a week of home care.
- Pus or discharge: The sore is weeping yellow or green fluid, which is a clear sign of a bacterial infection.
- Significant pain: The discomfort is more than mild and is interfering with your daily activities or sleep.
- Underlying health conditions: You have a condition that weakens your immune system, such as diabetes, or are undergoing treatments like chemotherapy.
Seek Urgent Medical Attention for These Red Flags:
Some symptoms can signal a more serious, fast-moving infection that requires immediate medical assessment to prevent it from spreading. Please visit your nearest Urgent Treatment Centre or A&E if you have a skin infection accompanied by:
- Rapidly spreading redness: The red area around the sore is expanding quickly, particularly if you see red streaks moving away from it. This can be a sign of cellulitis.
- Systemic symptoms: You develop a high fever, chills, or feel generally unwell and lethargic.
- Severe or disproportionate pain: The pain is extreme and seems much worse than the appearance of the infection would suggest.
- Location near the eye: Any sign of infection on the eyelid or close to the eye, or any infection causing significant facial swelling.
Ignoring these warning signs can allow an infection to spread into the bloodstream or deeper tissues. Prompt action is the most effective way to manage common skin infections and ensure your wellbeing. If you have concerns about a non-healing wound, especially following a hospital stay, understanding all potential causes is key. For more information on specific bacterial concerns, you can visit mrsatest.co.uk.
Diagnosis, Treatment, and Prevention Strategies
Understanding how common skin infections are diagnosed and managed is the first step toward effective recovery. If you suspect an infection, seeking a professional medical opinion from your GP is crucial for receiving an accurate diagnosis and the correct treatment plan. This ensures a swift and safe return to healthy skin.
How Are Skin Infections Diagnosed?
Most skin infections can be diagnosed through a simple physical examination of the affected area. To identify the precise cause, your doctor may take a small sample. This is often done with a skin scraping or a sterile swab, which is then sent to a laboratory for analysis. This process helps to pinpoint the specific bacterium, fungus, or virus responsible. For bacterial infections, a culture test can also be performed to check for antibiotic resistance. This is particularly important for identifying strains like MRSA, which require specific management. For concerns about MRSA, confidential home testing options are available for your peace of mind.
General Treatment Principles
Treatment is tailored to the type of organism causing the infection. While your doctor will prescribe the most appropriate course of action, general approaches include:
- Bacterial Infections: Typically treated with topical antibiotic creams for mild cases, or oral antibiotics for more widespread or severe infections.
- Fungal Infections: Addressed with over-the-counter or prescription antifungal creams, powders, or, in persistent cases, oral antifungal medication.
- Viral Infections: Many viral skin issues resolve with supportive care at home. For certain viruses, such as herpes simplex, antiviral medications may be prescribed to manage outbreaks.
- Parasitic Infections: These require medicated lotions or pills specifically designed to eliminate the parasites and their eggs, such as for scabies.
Beyond prescribed treatments for active infections, maintaining skin health often involves using high-quality supplies for aftercare and prevention. For those in the aesthetic and medical fields looking for professional-grade products, online retailers like Confidence Fillers offer a comprehensive range of supplies.
Simple Steps for Prevention
Good hygiene is the cornerstone of preventing future common skin infections. By incorporating a few simple habits into your daily routine, you can significantly reduce your risk:
- Wash your hands regularly with soap and warm water, especially after touching an infected area or being in public spaces.
- Keep wounds clean and covered. Clean any cuts, scrapes, or grazes thoroughly and apply a sterile bandage to protect them from bacteria.
- Avoid sharing personal items. Do not share towels, razors, clothing, or sports equipment that comes into direct contact with skin.
- Keep skin dry. Pay close attention to areas where skin folds, such as under the arms or in the groin, as moisture can encourage fungal and bacterial growth.
Navigating Skin Infections with Confidence
Understanding the landscape of common skin infections is the first and most critical step toward effective management and peace of mind. By learning to distinguish between bacterial, viral, and fungal types and recognising the key symptoms that warrant a doctor’s visit, you empower yourself to take swift, appropriate action. Prompt and accurate diagnosis is essential for successful treatment and preventing further complications.
For specific concerns about serious bacterial infections like MRSA, taking a proactive approach is vital. If you need clarity and assurance, you can test from the comfort of your own home. Explore our confidential at-home MRSA testing options. Our service provides fast PCR and standard culture tests processed by a trusted, UKAS-accredited laboratory partner. With discreet packaging and confidential results, you can get the answers you need with complete privacy.
Staying informed and utilising accessible diagnostic tools allows you to confidently protect your skin health.
Frequently Asked Questions
How can I tell if my skin infection is bacterial or fungal?
Differentiating between bacterial and fungal infections requires a clinical diagnosis, but there are general signs. Bacterial infections, like impetigo or cellulitis, often appear as red, warm, swollen areas, sometimes with pus or honey-coloured crusts. Fungal infections, such as ringworm, typically present as scaly, itchy patches, often in a ring shape or in skin folds. For an accurate diagnosis and the correct treatment, it is essential to consult your GP.
Can a skin infection go away on its own without treatment?
While very minor skin irritations may resolve, most true skin infections require medical treatment to prevent them from worsening or spreading. Untreated bacterial infections in particular can lead to more serious health complications. It is always the safest course of action to seek a professional medical opinion from your GP or a pharmacist if you suspect you have a skin infection, especially if symptoms persist or worsen over a few days.
How do I know if my skin infection is serious?
You should seek urgent medical attention if you notice signs of a serious infection. These red flags include rapidly spreading redness or red streaks extending from the area, severe or increasing pain, fever, chills, or feeling generally unwell. An infection that is near your eyes should also be treated as an emergency. In these situations, please contact NHS 111 or visit your nearest A&E for an immediate assessment.
What is the difference between cellulitis and a regular skin rash?
Cellulitis is a specific and deeper bacterial infection of the skin and underlying tissues. It presents as a red, swollen, hot, and tender area that can spread quickly. A rash is a more general term for any inflammation of the skin, which can be caused by many things, including allergies, viruses, or irritants. Unlike a simple rash, cellulitis is a serious condition that requires prompt antibiotic treatment from a healthcare professional.
Is MRSA considered a common skin infection?
Yes, MRSA (Methicillin-resistant Staphylococcus aureus) can cause several common skin infections, such as boils, abscesses, and cellulitis. While often associated with healthcare settings, it can also be acquired in the community. The key characteristic of MRSA is its resistance to certain widely used antibiotics, which makes a correct diagnosis essential for ensuring you receive an effective and targeted treatment plan from your doctor.
How can I stop a skin infection from spreading to other people?
Good hygiene is critical to prevent transmission. Keep the infected area clean and covered with a sterile dressing. Wash your hands thoroughly with soap and water after touching the area or changing the dressing. Do not share personal items such as towels, razors, flannels, or bedding until the infection has completely cleared. Following the full course of treatment prescribed by your GP is also essential to eradicate the infection.