The Complete Guide to Pre-Op Assessment MRSA Swabs: Why Timing and Accuracy Matter
Last Tuesday, Sarah discovered that her long-awaited knee surgery was being postponed indefinitely because her pre-op assessment mrsa swab results hadn’t reached the admissions team in time. For many patients across the UK, the fear of a last-minute cancellation is often more stressful than the operation itself. It’s a common frustration. You’ve prepared mentally and physically, yet a simple administrative delay or a slow laboratory turnaround stands in your way. You deserve to feel prepared and in control of your own health data.
We understand that you want your surgery to proceed safely without the anxiety of being a carrier or the uncertainty of NHS waiting lists. This guide explains exactly why MRSA screening is a mandatory safety requirement for UK surgical admissions. You’ll learn the critical differences between rapid PCR detection and traditional culture tests to help you meet your specific surgical deadline. We also provide a clear path to securing fast, confidential results from a UK-based, accredited laboratory. This ensures you can head into your procedure with total peace of mind.
Key Takeaways
- Understand why MRSA screening is a mandatory safety requirement for UK surgeries and the clinical difference between colonisation and infection.
- Compare traditional culture methods with rapid PCR technology to ensure your pre-op assessment mrsa swab provides accurate results within your surgical timeline.
- Learn the correct clinical techniques for performing a discreet at-home swab to ensure your samples are valid for UKAS-accredited laboratory testing.
- Discover the standard decolonisation protocols used to manage positive results, ensuring your operation can proceed safely and without unnecessary delay.
What is a Pre-Op Assessment MRSA Swab and Why is it Mandatory?
Preparing for surgery involves several safety checks designed to protect you while you’re in the hospital. A pre-op assessment mrsa swab is a routine part of preparing for surgery in the United Kingdom. It’s a simple test that identifies whether a specific type of bacteria is living on your skin before you enter the operating theatre. This bacteria, known as Methicillin-resistant Staphylococcus aureus, is a strain of common “staph” bacteria that has developed resistance to many standard antibiotics. Understanding What is MRSA? helps clarify why clinical teams are so diligent about screening before elective procedures.
For most people, carrying these bacteria isn’t a problem in daily life. However, the clinical environment of a hospital is different. Since 2010, the Department of Health has mandated that almost all patients undergoing elective admissions must be screened. This policy was introduced to lower the risk of hospital-acquired infections, which can complicate recovery and extend your stay. By identifying carriers early, the surgical team can provide a simple “decolonisation” treatment to clear the bacteria before your incision is made.
It’s vital to distinguish between two states: colonisation and infection. Most patients who test positive during a pre-op screen are merely colonised. MRSA colonisation is the presence of bacteria without active symptoms. In contrast, an infection occurs when those bacteria enter the body, perhaps through a surgical wound or a catheter, and cause symptoms like redness, swelling, or fever. The goal of the swab is to catch colonisation so it never turns into an infection.
The Risks of MRSA in a Surgical Environment
During surgery, your skin’s natural barrier is broken. This creates a direct pathway for any bacteria resting on your skin to enter your bloodstream or deep tissue. If MRSA is present, it can lead to a Surgical Site Infection (SSI). These infections are particularly difficult to treat because the bacteria don’t respond to the most common antibiotics, such as flucloxacillin. This resistance means doctors must use stronger, “last-resort” intravenous antibiotics, which often have more side effects and require a longer hospital stay. When metalwork like a prosthetic joint is involved, the bacteria can cling to the implant, making the infection nearly impossible to clear without further surgery.
Who Specifically Needs a Pre-Op Swab?
While screening is widespread, certain groups are prioritised due to the complexity of their procedures. If you’re undergoing orthopaedic surgery, such as a hip or knee replacement, a swab is mandatory because of the high risk associated with metalwork. Cardiac surgery and neurosurgery patients also face strict screening requirements because infections in the heart or brain carry severe consequences. You can learn more about the biology of these bacteria and why they behave this way by visiting our guide on What is MRSA? to better understand your results.
- Inpatients: If you’re staying overnight after your operation, you’ll almost certainly require a swab.
- Day Case Patients: Requirements vary, but if your procedure involves high-risk areas or implants, you’ll still be screened.
- Previous Carriers: If you’ve had MRSA in the past, hospitals will prioritise your pre-op assessment mrsa swab to ensure you’re clear before admission.
The screening process usually happens two to four weeks before your surgery date. This timeframe gives the hospital enough time to process the lab results and, if necessary, provide you with the antibacterial body wash and nasal cream needed to clear the bacteria. Being proactive about this step ensures your surgery goes ahead as planned without last-minute cancellations.
The Science of Screening: How MRSA is Detected
A pre-op assessment mrsa swab is a vital step in surgical preparation. It isn’t just a simple wipe; it’s a targeted search for specific bacteria that could cause post-operative complications. Clinical teams focus on areas where bacteria thrive to ensure nothing is missed before you enter the operating theatre. This process identifies “colonisation,” which means the bacteria are living on your skin without causing an active infection.
Common Swab Sites and Their Importance
Scientists have identified specific “reservoirs” on the human body where Staphylococcus aureus prefers to live. The nostrils are the primary site. Research indicates that roughly 30% of the healthy population carry Staph bacteria in their nose at any given time. Because the nasal passage is warm and moist, it provides the perfect environment for bacterial colonies to grow without causing symptoms.
The groin and axilla (armpit) are the next most critical areas. These regions have a higher density of sweat glands and skin folds. These folds create micro-climates that support bacterial survival even after regular washing. By testing these three distinct sites, clinicians can increase the likelihood of detecting colonisation by up to 95%. This thorough approach ensures that your pre-op MRSA screening provides a complete picture of your skin flora.
Understanding Laboratory Accuracy
Once your swabs are taken, they’re placed in a transport medium. This gel-like substance stabilises the sample, preventing the bacteria from dying or overgrowing during the journey to the lab. Accuracy depends entirely on using UKAS-accredited facilities. These laboratories meet rigorous ISO 15189 standards, ensuring that every result is both reliable and legally defensible for surgical clearance. It’s the same level of scrutiny applied to samples taken within an NHS hospital.
This reliance on specialist, accredited services for peace of mind is common in other major life events too. For instance, when navigating the complexities of a property purchase, you can discover Local Authority Search Network Ltd (Mynlis) for essential conveyancing searches and reports.
In the lab, clinical scientists use two main metrics to evaluate your sample:
- Sensitivity: This measures how well the test identifies people who actually have MRSA. High sensitivity means fewer “false negatives.”
- Specificity: This measures the test’s ability to correctly identify those without the bacteria. High specificity, often exceeding 98% in modern labs, ensures you aren’t treated for an infection you don’t have.
Modern labs often use PCR (Polymerase Chain Reaction) technology to look for the mecA gene. This specific gene is what makes standard Staph resistant to methicillin. While traditional cultures take 48 hours to grow, PCR can deliver results in under 24 hours. If you’re looking for a fast, reliable way to tick this off your surgical checklist, you can order a professional testing kit to use at home.
A single swab might miss a low-level colonisation. That’s why your pre-op assessment mrsa swab protocol often requires multiple samples from different body sites. This redundancy acts as a safety net. It accounts for the fact that bacteria aren’t always evenly distributed across the skin. By being thorough at this stage, the surgical team can proceed with confidence, knowing they’ve minimised the risk of a hospital-acquired infection to the lowest possible level.
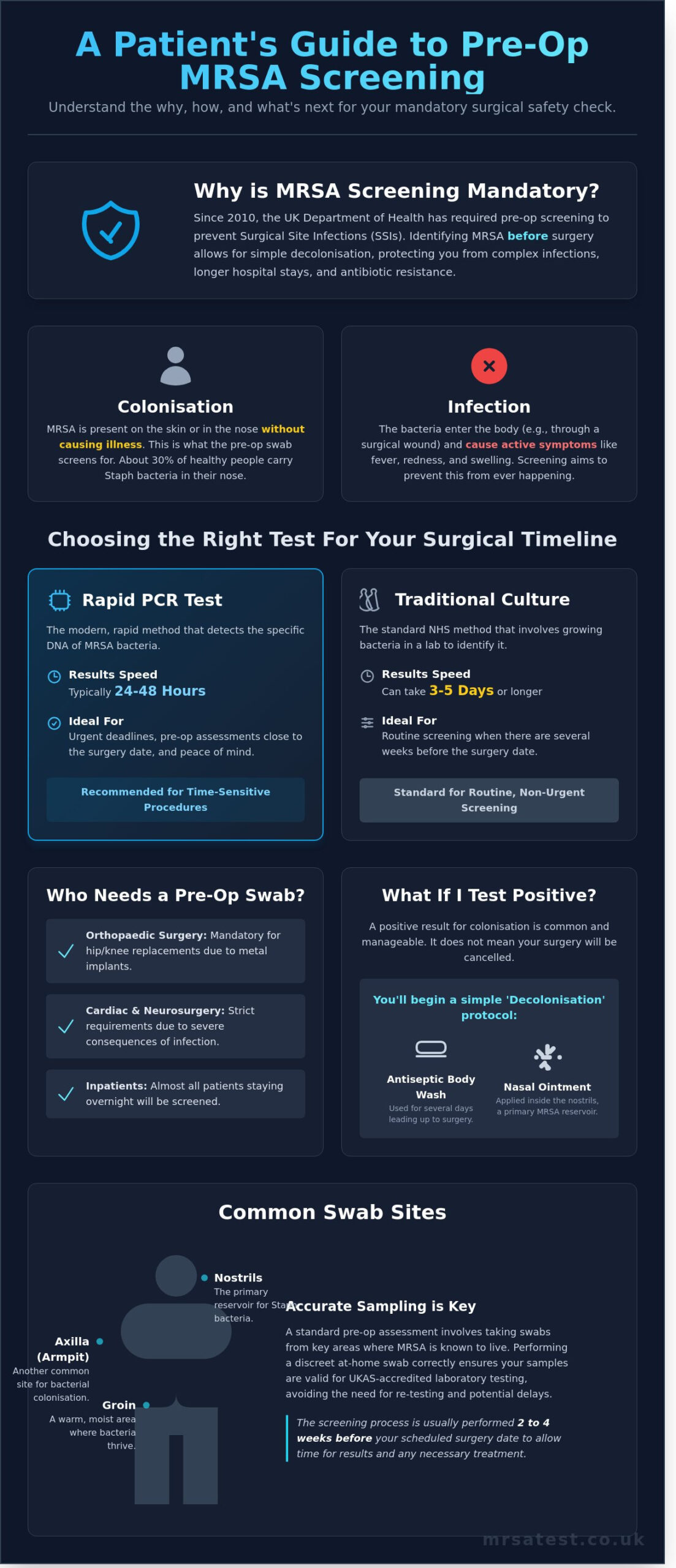
Comparing Testing Methods: PCR vs. Culture for Surgery Prep
When you attend your pre-op assessment mrsa swab, the laboratory processes your samples using one of two primary technologies. Choosing between a traditional culture and a rapid PCR test depends entirely on your surgical timeline and the specific requirements of your hospital. Both methods are highly accurate, but they operate on different biological principles and offer vastly different turnaround times.
The culture method is the traditional approach used by many NHS trusts. It involves placing your swab samples onto a nutrient-rich agar plate and incubating them at 37°C to encourage bacterial growth. Scientists then wait for visible colonies to form. This process typically takes between 48 and 72 hours. While it’s a reliable way to confirm the presence of bacteria, the wait can be stressful if your surgery date is fast approaching. A Clinical Review of Pre-Op MRSA Screening shows that while culture is effective, the delay in results can complicate the management of surgical lists.
PCR (Polymerase Chain Reaction) testing takes a molecular approach. Instead of waiting for bacteria to grow, it searches for specific genetic sequences. PCR testing detects bacterial DNA, allowing for results within one working day. Because this method identifies the mecA gene responsible for methicillin resistance almost instantly, it’s the gold standard for patients who need answers quickly. For any operation scheduled in the next seven to ten days, the speed of a PCR test provides a vital safety net.
The Time Factor: Avoiding Surgical Cancellation
Timing is the most frequent reason for MRSA-related surgical delays in the UK. If you receive a positive result via a slow culture test just 48 hours before your procedure, there simply isn’t enough time to clear the bacteria. You need a 5-day decolonisation window to complete the prescribed antiseptic washes and nasal creams before you can safely enter the operating theatre. If a late NHS result shows colonisation, your theatre slot will likely be reassigned to another patient to prevent the surgical team from standing idle. Using a rapid PCR test ensures you have your results in time to complete any necessary treatment without risking your place on the list.
Culture Testing: The Gold Standard for Sensitivity
Standard culture tests remain the preferred choice when your surgical timeline isn’t urgent. If your operation is more than three weeks away, the 72-hour wait is less of a concern. The main benefit of this method is the ability to perform “sensitivity testing.” By growing the live bacteria, microbiologists can test it against various antibiotics to see which ones are most effective. This provides a detailed map of resistance patterns that can be invaluable for your post-operative care. You can find a deeper technical breakdown of these processes in our guide to the MRSA Culture vs PCR Test.
When evaluating cost versus speed, it’s helpful to look at the broader picture. A PCR test generally costs about £30 to £50 more than a standard culture test. However, when you consider that a cancelled private surgery can result in lost deposits or significant administrative fees, the investment in speed is often the most economical choice. Most patients find that the peace of mind provided by a 24-hour result far outweighs the modest price difference. If you’re managing your own pre-op assessment mrsa swab requirements, always check your hospital’s specific deadline before choosing your testing method.
Step-by-Step: How to Perform Your Pre-Op MRSA Swab at Home
Performing your pre-op assessment mrsa swab correctly ensures your surgery proceeds without delay. Start by selecting a well-lit area, such as a bathroom, and clearing a clean surface. Wash your hands thoroughly with soap and water for at least 20 seconds. Lay out the kit contents: the sterile swab, the transport tube containing the buffer liquid, and the laboratory request form. Check the expiry date on the swab packaging; 99% of our kits are dispatched with at least 12 months of shelf life remaining. Accurate results depend on preventing outside bacteria from entering the sample, so don’t touch the swab tip against your hands, the counter, or any household surfaces.
Nasal Swab Technique
Carefully peel back the paper wrapper to reveal the swab handle. Insert the soft tip approximately 2cm into your first nostril. You don’t need to go deep enough to cause discomfort, but the tip must make contact with the internal mucosal lining. Rotate the swab firmly against the inside wall five times. Repeat this exact process in the second nostril using the same swab. This 10-second procedure ensures the tip is sufficiently saturated with skin cells and secretions. If the swab feels dry, it may not collect enough material for the lab to process accurately.
Groin and Axilla Swabbing
The axilla (armpit) and groin are primary sites for MRSA colonisation due to the warmth and moisture of skin folds. For the axilla, rub the swab tip back and forth across the skin fold for 5 seconds using firm but gentle pressure. Repeat this for the other armpit. For the groin area, target the crease where the inner thigh meets the torso. If your specific instructions require a single swab for all sites, always follow the “top-to-bottom” sequence: nose first, then axilla, and finally the groin. This specific order is a clinical standard that prevents the transfer of bacteria from the lower body to the nasal passages during the sampling process.
The Return Process
Once you’ve finished sampling, place the swab into the plastic transport tube and push the cap until it clicks shut. This seal prevents the buffer liquid from leaking during transit. It’s vital to write your full name, date of birth, and the “Collection Date” on the tube label. Data from UK clinical settings shows that approximately 12% of home samples face processing delays because the collection date was omitted. Place the tube into the protective biohazard bag, then into the provided unbranded mailing box. Use the prepaid Royal Mail Tracked 24 label to ensure the kit reaches our UKAS-accredited laboratory within 24 hours. Our packaging is entirely discreet; there are no external markings indicating the nature of the test, protecting your medical privacy throughout the delivery process.
Managing a Positive Result Before Your Operation
Receiving a positive result from your pre-op assessment mrsa swab can feel alarming, but it isn’t a reason to panic. It’s vital to understand that a positive result doesn’t mean you’re ill or that you have an active infection. Instead, it means you’re “colonised.” This indicates the bacteria are living harmlessly on your skin or inside your nose. While this causes no issues in daily life, these bacteria can pose a risk if they enter a surgical wound. By identifying this status early, you can take simple steps to clear the bacteria before your procedure begins.
The primary goal of screening is safety. If your test returns a positive result, your surgical team will simply initiate a “decolonisation” process. This is a routine preventative measure used across the NHS and private hospitals to protect patients from post-operative complications. Knowing your status in advance puts you in control, allowing you to complete treatment in the comfort of your home rather than facing a last-minute cancellation at the hospital gates.
The Decolonisation Programme
The standard UK protocol for clearing MRSA is a straightforward 5-day routine. You’ll typically be prescribed two specific treatments: a nasal ointment and an antiseptic body wash. The nasal cream is usually 2% Mupirocin, often sold under the brand name Bactroban. You’ll need to apply a small amount to the inside of each nostril three times a day using your little finger or a cotton bud. This targets the area where the bacteria most commonly reside.
Alongside the nasal cream, you’ll use an antiseptic wash such as 4% Chlorhexidine, commonly known as Hibiscrub. You should use this as a liquid soap in the shower once a day for the full five days. It’s important to pay particular attention to areas like your armpits, groin, and navel. To make the treatment as effective as possible, follow these hygiene steps:
- Wash your bedding and towels at 60°C on the first and last day of the treatment to kill any lingering bacteria.
- Use a fresh flannel or sponge for every wash and don’t share towels with other members of your household.
- Change into clean clothes and pyjamas every day during the 5-day programme.
- Avoid using standard moisturising lotions or perfumes immediately after washing, as these can sometimes interfere with the antiseptic’s action.
Coordinating with Your Surgical Team
If you’ve opted for private screening, you should provide the UKAS-accredited lab report to your Pre-Operative Assessment Clinic (POAC) as soon as you receive it. Hospital staff are accustomed to managing these results and will appreciate the early notice. Providing this documentation allows the clinical team to update your records and confirm that you’ve followed the correct decolonisation steps. This transparency ensures there are no surprises on the morning of your surgery.
Early detection via a private pre-op assessment mrsa swab is often more convenient than waiting for a hospital appointment. If you discover a positive result two weeks before your operation, you have ample time to complete the 5-day wash routine and perform a retest. Most hospitals require you to wait at least 48 hours after finishing the treatment before taking a follow-up swab. This gap ensures the antiseptic has cleared, providing an accurate reading to confirm you are clear for the theatre.
Don’t leave your surgical safety to the last minute. Order your fast-tracked MRSA test kit today to ensure you have the time and peace of mind needed for a successful recovery.
Secure Your Surgery Date with Reliable Screening
Preparing for an operation is stressful enough without the worry of last-minute cancellations. Understanding the role of your pre-op assessment mrsa swab is the first step toward a successful recovery. Whether you choose a standard culture or a rapid PCR test, accuracy is vital for hospital safety. By testing early, you provide yourself with a necessary window to manage a positive result without delaying your procedure.
You don’t need to wait for a GP appointment to get started. Our service provides 100% confidential and discreet home delivery, allowing you to collect your sample in private. Every test is processed in UKAS-accredited UK laboratories to ensure clinical precision. If you’re on a tight schedule, our PCR rapid test option provides molecular detection results in as little as 24 hours.
Take the uncertainty out of your surgical preparation. Order Your Private Pre-Op MRSA Test Kit Now and gain the peace of mind that comes with professional, fast, and secure screening. We’re here to help you move forward with your treatment safely.
Frequently Asked Questions
How long does an MRSA swab take to come back before surgery?
A standard culture test usually takes 48 to 72 hours for results to be processed by a laboratory. If you choose an MRSA PCR rapid test, you’ll often receive your results in as little as 24 hours. It’s best to complete your pre-op assessment mrsa swab at least 7 days before your scheduled surgery. This timeframe ensures all results are confirmed and any necessary decolonisation treatment can begin without delaying your procedure.
What happens if I test positive for MRSA at my pre-op assessment?
If you test positive, your clinical team will prescribe a decolonisation treatment kit to clear the bacteria. This typically includes a 2% mupirocin nasal ointment applied three times daily and a 4% chlorhexidine body wash used once a day for 5 days. These steps reduce the risk of a surgical site infection by removing the bacteria from your skin and nose. You’ll usually need a follow-up swab to confirm the treatment worked.
Can I still have my operation if I have MRSA?
Yes, you can still have your operation, but it’s often delayed by 5 to 7 days to allow for decolonisation treatment. Hospitals frequently place MRSA-positive patients at the end of the theatre list to allow for deep cleaning of the room. You might also receive specific intravenous antibiotics, such as vancomycin, during the procedure itself. Your surgeon will decide the safest timing based on the urgency of your specific surgery and clinical needs.
How do I do an MRSA swab at home for a pre-op?
Taking a pre-op assessment mrsa swab at home is a simple process using a sterile kit. You’ll need to moisten the swab with the provided liquid and rotate it inside both nostrils for 5 seconds each. You then use separate swabs for your throat, armpits, and groin area as instructed. Once finished, place the swabs into the transport tubes and send them to our UKAS-accredited laboratory using the provided discreet, pre-paid packaging for fast analysis.
Why do they swab the groin for MRSA?
Clinical studies show that MRSA bacteria frequently colonise warm, moist areas of the body like the groin and armpits. Up to 15% of people carry MRSA in these skin folds even if the bacteria isn’t present in their nose. Swabbing the groin ensures a more accurate screening process. This thorough approach reduces the risk of bacteria entering a surgical wound, which is vital for preventing post-operative complications and ensuring a safe recovery.
Is the MRSA PCR test more accurate than a culture test?
Both tests are highly reliable, but the PCR test is faster and offers a sensitivity rate of over 98%. While a culture test takes 3 days to grow and identify bacteria, the PCR method detects MRSA DNA in just 24 hours. This speed is helpful if your surgery is scheduled soon. However, culture tests are still valuable because they allow laboratories to test which specific antibiotics will effectively kill the bacteria if an infection occurs.
How much does a private MRSA pre-op swab cost in the UK?
A private MRSA culture test in the UK typically costs around £49, while a rapid PCR test is priced at approximately £89. These prices include the home test kit, laboratory analysis in a UKAS-accredited facility, and your official results certificate. Choosing a private option provides a fast and discreet way to complete your screening without waiting for a hospital appointment. This helps ensure your surgery stays on schedule and provides peace of mind.
Can I treat MRSA myself before my hospital appointment?
You shouldn’t attempt to treat MRSA with over-the-counter creams or standard soaps because they won’t clear the colonisation. Effective decolonisation requires specific prescription-only products like 2% mupirocin nasal ointment. Using the wrong products can lead to antibiotic resistance and won’t satisfy hospital safety requirements. If you’re concerned, using a private screening service allows you to identify the bacteria early. You can then obtain the correct clinical treatment from a doctor before your surgery date.







